Poverty is not something new that just appeared in the United States. It’s been present for generations. And, in those days, especially in small towns. The local town doctor was a very busy professional making house calls to help residents and neighbors with ills, conditions, injuries, and chronic sickness.
In the last few decades, however, the push towards health by insurance and processing of the sick through institutional systems did away with the visiting doctor for years, slowly creating a system of financial haves and have-nots. Those who could afford insurance obtained health coverage. Those who could not end up never visiting the doctor at all or relied on a free clinic here or there. By the 2000s, this problem was widespread as evidenced by the thousands who showed up for special dental and health check clinics organized by volunteer doctors.
Bring Health Back to People Where They Are
In the push to reach out and reverse the above trend, mobile health clinics started to be created, first as small local projects and then as larger outreach programs funded by government grants and non-profit support. They have also realized a role in disaster response as well. The concept is simple – bring health to the people. With a mobile unit, a doctor and support staff move from location to location where the poor live and provide free or low-cost direct health service. The impact has been significant as it 1) eliminates the distance problem blocking people from getting to health services, 2) avoids the cost problem, and 3) provides real health checkups, exams, and medicine for people who really need it.
Medical Flexibility Means Streamlining
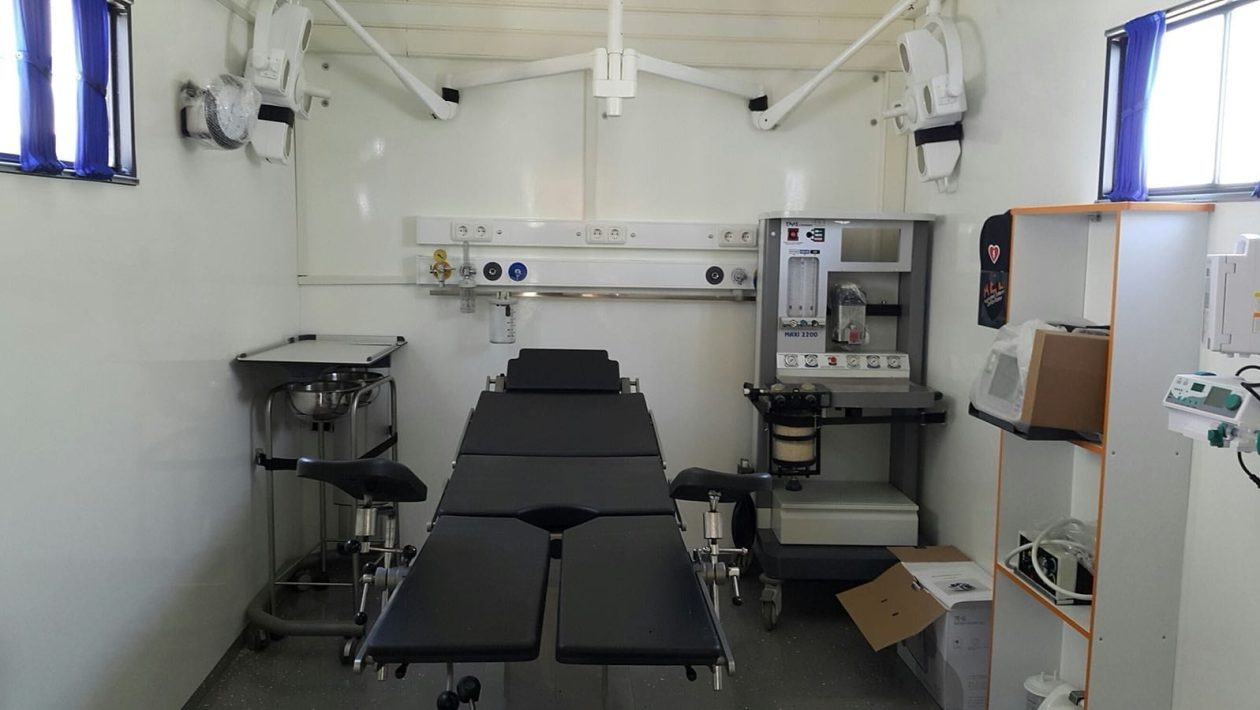
The effectiveness of mobile clinics starts with their equipment. The tools and containment need to be both compact and functional. There is only so much room available in a trailer redesigned to be a clinical office, and it also needs to be able to store supplies, hazardous materials removal, and workspace for the doctor and patient. So, the standard approach with clinical equipment doesn’t automatically work. Some tools have to be crossed out because they simply aren’t compatible with the tight space. On the other hand, choices like C-arm designs (minicarm.com) make considerable sense, being compact and effective for treatment in a mobile system.
The ultimate utility of mobile health clinics depends on how well they reach out as well as how much funding can be put behind them to keep going. After all, these programs are not intended to be profitable; they are outreach to those who can’t afford health otherwise. That said, as long as clinics are supported, smart medical equipment can contribute to making a difference across the U.S. as a result.